 [Update: This is one of my first posts on this blog, and it’s also one of my most popular. Too bad it’s a long post that isn’t the clearest. So here’s a shortened and clarified version.]
[Update: This is one of my first posts on this blog, and it’s also one of my most popular. Too bad it’s a long post that isn’t the clearest. So here’s a shortened and clarified version.]
On Wednesday, I went to the Health System Reform Task Force meeting at the Utah State Capital building. I recently learned that most governmental meetings are open to the public, so you can go to them whenever you want! During the meeting, they often have someone present some kind of informational presentation to help them get a better idea of what’s going on in healthcare. Last month, a physician from Intermountain Health Care presented on prescription drug abuse in Utah. (It’s pretty bad, if you didn’t know. Actually, I think he said that Utah is the worst state for prescription drug overdose fatalities.) This month, a physician talked about some “demonstration project” he’s leading to improve pediatric care in Utah. It was pretty interesting, but the most interesting part was when he said the following: (These are direct quotes transcribed from the audio recording of the meeting.)
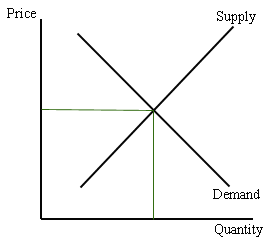
“Supply and demand, which in most markets works perfectly, doesn’t work so well in healthcare. The demand for healthcare really sees no limit, especially if cost is not a factor for the consumer, and that is the case, of course, in most third-party payment situations. But I think it’s also the case in situations where life is in the balance. It’s hard to put a limit on how much you’re going to demand. And also, I think consumers can’t adequately evaluate their options. Shopping around for a physician, shopping around for a surgeon is not easy. Shopping around for emergency care when you really need it is impossible. So the ability really to be a wise and educated consumer and make conscientious choices is difficult. And also the supply of physicians and providers is not driven by normal market forces. We see a lot of increasing specialization for reasons that aren’t necessarily fitting with the supply-demand curve. Specialization is driven by income, especially because specialists make considerably more in most cases than primary care physicians.”
This got me thinking, and I started evaluating his statements and typing notes on my phone. Then I was surprised when the senate chair of the committee challenged him on it after the presentation.
“I just had one comment, and maybe you could clarify if it was an intended comment. You mentioned in your presentation that supply and demand did not apply.”
Physician’s interjection: “I didn’t say it did not apply, I said it didn’t work, like it does in most markets. So, just to clarify your question.”
The Senate Chair continued, “Well, the comment I have on that is that supply and demand function, whether we want it to. It functions, it’s natural law, whether we want it to or not. We can try and interfere with it, but, a lot of the things, I believe I could demonstrate a lot of the problems you presented there are a result of interfering with supply and demand. And so, the idea that it doesn’t function and we can try and overcome it, I think that’s a basis for failure in the long run, that we’re just going to have to control healthcare more and more because if supply and demand is going to function, and its results are, the unintended consequences we’re trying to control. So we continue to regulate more and more. . .”
And the physician’s response, “I’m probably not sophisticated enough economically to speak to the question, but I hear what you’re saying and I agree.”
At this point, I almost raised my hand, walked to the microphone, and answered his question. I should have. But I wasn’t sure if I was allowed to do that, so I hesitated and missed the opportunity. That means I get to say here what I would have said there:
My honorable legislators, supply and demand carry with them a few assumptions. When those assumptions are violated, supply and demand don’t work as well as we would expect. Two key assumptions are violated by our current healthcare system. The first is that consumers have price/quality information so they can shop around for the best value. The second is that consumers actually pay the price of what they buy.
The First Broken Assumption. Let’s think about an example of digital cameras. Without important information like how much a camera costs or how many mega-pixels it has and how many times zoom it can do, how do consumers choose the best value? They can’t! And thus, there’s not much incentive for camera manufacturers to take risks to improve cameras because it won’t help them make more money. Innovation is stifled without that incentive. To bring this back to healthcare, why would a doctor’s office make an innovation like install an electronic medical record that would temporarily disrupt process flows and require a large upfront cost if it won’t help convince more patients to come?
The Second Broken Assumption. This is a tricky one. Yes, consumers pay the full cost for their healthcare–they have already done it through insurance premiums or reduced salary. But they don’t see that full price directly like it’s coming straight out of their wallet, so they don’t perceive that they’re paying the price. Thus, they don’t care so much what the price is. This inflates demand in a big way! Think about the man whose father is about to die. He’ll tell the doctor to do whatever it takes to keep the father alive, but how willing would he be to do that if the man knew he was going to have to pay $600,000 right out of his own bank account?
That’s what I would have said. It’s almost exactly what the physician said, but I don’t think he understood it quite well enough to realize that the things he was talking about were actually just the broken assumptions of supply and demand in healthcare.
After I thought this, I understood a part of the health bill in an entirely new light. It’s requiring states to form these “health insurance exchanges” that are essentially websites that list all the state’s available insurance plans, their prices, and their benefit packages. What will this do? Help people know prices! Help people know value! It’s a way to solve the first broken assumption.
There are many critics of “market-driven healthcare.” They say it has never worked in the U.S., so how can advocates of it be so ridiculous? Well, I guess now we know why it has never worked, and now all you conservatives can understand your argument for less government in healthcare, assuming (as does the Senate Chair for the Health Reform Task Force) that it’s the government that is causing those assumptions to be broken.

We are pleased that you are getting into the nitty-gritty of the health care debate. We agree with you that it is a thorny problem — the more we learn about it the better.
Lots of love, Jay and June
The overall idea is moving toward perfect information, which includes not only price (as you mentioned), but also quality and satisfaction. These two other factors contribute to one’s decision, quality less than satisfaction, but they both play a significant role. Pertaining to quality, most patients assume a certain degree of competence in their physician, and as such, remain unaware of quality measures. What patients care more about is how the nurse treats me, or whether or not my hot food was really hot and my cold food stayed cold. Hence, many hospitals release quality information along with HCAHPS results.
Well said, TJ.
The economic jargon is market failure occurs when there is “information asymmetry” or, as Alex said, when there isn’t “perfect information.”
The U.S. healthcare system is full of information asymmetry because of the other problem you pointed out, which is that true costs are veiled and often passed on to someone else. As soon as health consumption decisions became artificially cheap (or seemingly so)–monthly premiums taken pre-tax, before paychecks are cut and you pay a small co-pay–we destroyed the incentive for individuals to demand good information. After a few decades, we are where we are now.
Markets have natural checks and balances–limited supply and limited willingness to pay–but our system made it much easier for everyone “to pay,” thus, our “market” is distorted.
As you’ve suggested, solutions must a) create and reward information gathering, b) move the full cost of transactions more into the hands and mind and wallet of the consumer.
Perhaps the insurance exchange websites will help a), I’m still waiting on a Google/Wikipedia/digital cloud/social network kind of solution; but a relatively successfu solution for b) are high deductible plans paired with health savings accounts.
Miss you guys and BYU-HMA!
Nat, thanks for adding an element of sophistication that I somewhat avoided. The terms for these things are important, since that’s what everyone will see when they’re reading a well-written piece on health policy.
I haven’t much looked into the high-deductible plans yet, but they conceptually make sense that insurance should only be used for catastrophes, not for minor routine things. The trouble I haven’t been able to reconcile yet is whether the culture of America would adapt well to the alien idea of actually saving up for something that you’re not sure will happen in the future (i.e., a health catastrophe). If people don’t save up, then does that mean providers are forced to provide more charity care, thus increasing the costs they have to charge everyone else who actually did what they were supposed to do and saved up for that unexpected triple bypass?
From my experience working in Account Management in the health care industry managing very large company group plans, it’s obvious your normal supply and demand theory doesn’t fit. In our industry there are many, many conversations with our clients surrounding educating their employees to essentially “train” them to think like normal consumers when it comes to using their group health benefits. I work at a very large Health Care company and we have many resources that provide price comparison and provider/service quality ratings for employees to shop around. At minimum these resources include online resources, as well as telephonic resources. The challenge for us is the very rich benefits and money that these large companies are willing to spend in health care. And, they do so for various reasons, the main one is competition in recruiting and retaining employees in certain competitive industries such as Oil and Gas. In my opinion employees have the price and quality info available to them to compare and shop around, even in our smaller markets for our Clients who may only employee 100 people. But it’s a hard battle to fight when all the employee has to do is pay a $20 copay for treatment and the Client is willing to shell out the millions of dollars it cost to pay for the service. It’s like we play tug-of-war with these Clients. They need to provide the quality benefits needed to keep the employees they have, and we do all that we can during our Quarterly and Annual meetings to try and convince them where they can cut back and reduce utilization, and have their employees think like a normal consumers with their heatlh care benefits, as if they would when they go grocery shopping. It’s a very, very tough battle my friend! Take it from an insider.
Wes, your experience you describe tells me that incentives rule. If someone only has to pay a $20 copay regardless of which doctor they see, who would even bother to look at the full prices? People only care about what they’re personally responsible for. I think that’s why employers are starting to get smart and do things that force employees to be a little more connected to the total price, including multi-tiered insurance, reference pricing, and high-deductible plans. Check out this interesting brief on reference pricing: http://www.catalyzepaymentreform.org/uploads/CPR_Action_Brief_Reference_Pricing.pdf
It’s interesting you mention those things, especially Reference Based Pricing. Our clients have the opportunity to take advantage of these features/products. Some choose to explore those options, some are handicapped by their different Union groups, some will not even consider these options because of industry competition for employees. A National Accounts client looks to us to save the company money but will not consider changes that will matter from a claims and utilization prospective so we have to try and be creative with our internal programs that focus on these things that are unique to a client and hope it’s enough to make a difference. Sometimes we’re successful, sometimes not. Sometimes it’s just a matter of negotiating each year’s administrative fee. Every client would love it if we could keep their admin fee flat year over year but that’s impossible and will never happen, they know that as much as we know that. I guess bottom line is, as a company we do all we can to provide various options and avenues for our National Accounts clients but it is ultimately their decision.
I am surprised you say that some clients will not consider options like reference-based pricing due to competition for employees. I am making 2 assumptions:
1. Total Compensation = Salary + Benefits
2. Most new employees would be swayed more by a higher salary offered than a more generous benefits package, especially because comparing benefits from one potential employer to another is much harder than comparing the salaries they’re offering.
With these two things in mind, look what reference-based pricing would tend to do: (a) it would shift some of the compensation from benefits to salary by increasing out-of-pocket health spending (a pretty popular thing these days what with the rapid spread of high-deductible plans) and (b) it would lower the cost of the benefits the employer is offering, which savings could then easily be added to the salary they’re offering, thus increasing total compensation.
The potential employee then gets a no-brainer offer from this employer because, compared to his other offers, the salary is higher and the benefits are mostly indistinguishable.